For individuals with acute or chronic end-stage liver disease, liver transplantation is a highly beneficial operation. Previously, liver transplantation was considered a last resort for individuals suffering from advanced liver disease. Early mortality was quite high because patients were in such poor condition at the time of surgery. Although survival rates have improved significantly over time, there are still some issues that need to be addressed. Despite all the surgical, medical, and technological developments, liver transplantation is still a complicated process with high morbidity and mortality.
How does the liver work?
The liver is the main internal organ of the body and is essential for several key tasks. The liver is essential for the survival of a human being and its loss cannot be replaced. The liver performs several important tasks, including:
1. Formation of bile juice, a chemical mixture that is necessary for digestion.
2. Help break down food so it can be converted into energy.
3. Filtering and removing dangerous chemicals from the bloodstream.
4. compounds that fight infection are created.
5. Production of substances that help blood clotting.
6. Vitamins, iron, and other important chemicals are stored.
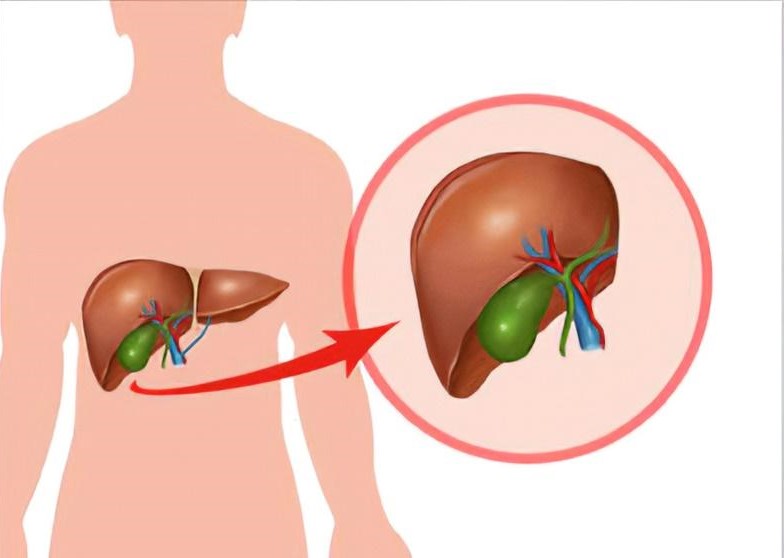
What is the significance of liver transport?
A liver transplant is a difficult medical operation that involves removing a diseased liver and replacing it with a normal one. This treatment has been performed for over 38 years. Many people who have had surgery go on to live completely normal lives afterward.
When a patient’s liver does not perform important functions and standard medical treatment fails to restore function, a liver transplant is performed. Liver failure can be caused by several factors. Liver scarring or liver cirrhosis, on the other hand, is the most typical indicator that a patient needs a liver transplant. Cirrhosis of the liver can be caused by several factors such as:
1. Alcoholic liver disease
2. Fatty liver
3. Hepatitis B
4. Hepatitis C
5. Genetically transmitted disease
6. Autoimmune liver disease
7. Except for cirrhosis of the liver, liver cancer, acute liver failure, and bile duct disease may also require transplantation.
Risks of a liver transplant
A liver transplant can result in several problems, some of which may develop immediately after surgery and others which may occur later. They are divided into two categories: acute and long-term problems.
Immediate effects:
The following are some of the immediate or short-term consequences of a liver transplant:
Technical problems: Arterial problems, especially thrombosis, are one of the most common transplant complications.
Health problems: As liver function gradually improves, the patient may develop complications. Under such circumstances, the patient’s stay in the ICU is prolonged and the probability of death increases. Neurological respiratory problems, kidney problems, and hemodynamic changes are among the most common health problems that can develop after donation.
Infections: Infections are a serious short-term problem that can occur after a transplant. Anti-rejection drugs increase the risk of infection by suppressing the immune system and preventing it from rejecting the new liver. This problem improves over time and most infections can be treated immediately.
Rejection: Unless anti-rejection drugs are given, the immune system will always reject the transplanted liver. Because the immune system cannot tell the difference between a transplanted liver and unwanted bacteria and viruses, this happens. Anti-rejection drugs are given to minimize the risk of rejection.
Liver graft dysfunction: Premature graft dysfunction can be caused by the following situations:
1. The graft itself causes problems such as liver rejection, nonspecific cholestatic syndrome, and graft failure or dysfunction.
2. The surgical approach may cause vascular or arterial problems, as well as poor drainage of the suprahepatic veins and portal thrombosis.
3. Infection or drug-related liver damage are two other possibilities.
Long-term effects:
In the past, liver transplantation was considered an experimental treatment and was used only as a last resort for patients in life-threatening situations. Long-term problems were not the main concern back then. Nevertheless, as the probability of survival increases, more emphasis is placed on long-term problems that are closely related to immunosuppressive treatment. Chronic renal failure, diabetes mellitus, dyslipidemia, obesity, systemic arterial hypertension, bone or neurological problems, and de novo tumor formation are the most common consequences that appear within several years of surgery.
Chronic rejection: This usually does not occur until 6 months after the transplant. Although the reason is unknown, there is still a chance that the liver will be rejected by the body.
Renal failure: The use of calcineurin inhibitors after transplantation is associated with chronic renal failure. The frequency of the problem varies depending on the parameters used to identify it and the methodology used to measure renal function.
Arterial hypertension: Arterial hypertension is one of the most common problems in liver transplant patients after surgery, with an incidence of 50-70 percent in the first months. However, as the dose of immunosuppressive drugs is reduced, it continues to decrease.
Diabetes Mellitus: Some people develop diabetes mellitus after donation. The likelihood of this happening depends on the length of time since the transplant and especially on the immunosuppressive drugs used.
Osteopenia: Osteopenia, a condition where the bones become weaker than usual, is common in those who have severe chronic liver disease. After liver transplantation, approximately 20-40% of patients may experience atraumatic bone fractures. The most common sites of these fractures are the vertebrae and ribs.
Obesity: Obesity has a hazard ratio of 15-40 percent in the first year after surgery when patients gain the most weight. It is among the most common long-term consequences.
Despite advances in the medical and surgical fields, liver transplantation is still a complicated medical process with both short- and long-term risks. Still, survival rates for the procedure have improved, and most problems are treatable.